CASE PRESENTATION
Lichen spinulosus in a black patient. Case report
Liquen Espinuloso en un paciente de piel negra. Presentación de caso
Alvaro Rojas Mora 1* https://orcid.org/0000-0001-6805-5364
Graciela Fundora Guerra 1 https://orcid.org/0009-0000-9273-0403
Isandra Alfonso Graña 1 https://orcid.org/0009-0009-8838-1963
Aylet Pérez-López 1 https://orcid.org/0000-0003-4629-9995
1 Calixto García General University Hospital. Havana, Cuba.
* Corresponding author: alvarorojasmorapiel@gmail.com
Received: 03/02/2026
Accepted: 01/04/2026
Published: 04/04/2026
How to cite this article: Rojas-Mora A; Fundora-Guerra G; Alfonso-Graña I; Pérez-López A. Lichen spinulosus in a black patient. Case report. MedEst. [Internet]. 2026 [cited access date]; 6:e522. Available in: https://revmedest.sld.cu/index.php/medest/article/view/522
ABSTRACT
Introduction: lichen spinulosus is a rare dermatosis characterized by plaques of follicular papules with central horny spines, giving them a sandpaper-like texture. Although its classic presentation is well documented in the literature, reports describing this entity in patients with darker skin tones are scarce.
Objective: to present a clinical case of lichen spinulosus in a black patient.
Case presentation: a 28-year-old male patient with a history of bronchial asthma presented with lesions on his back that had been present for two months. Physical examination revealed multiple plaques composed of follicular papules with central horny spines, which were slightly pruritic and had a rough texture. The skin biopsy showed dilated pilosebaceous follicles with keratin plugs and mild perifollicular lymphocytic infiltrate, findings consistent with lichen spinulosus. Treatment consisted of adapalene gel every other night and 10% urea cream daily. After 8 weeks, complete resolution of the lesions and recovery of normal skin texture were observed.
Conclusions: this case confirms that the classic clinical manifestations of lichen spinulosus persist in Black skin and that combined treatment with retinoids and topical keratolytic agents is effective. The importance of considering this dermatosis in higher phototypes, where reports are scarce, is highlighted.
Keywords: Lichen Spinulosus, Keratosis Pilaris, Black Skin, High Phototype, Topical Retinoids.
RESUMEN
Introducción: el liquen espinuloso es una dermatosis infrecuente caracterizada por placas de pápulas foliculares con espinas córneas centrales, que le confieren una textura similar al papel de lija. Aunque su presentación clásica está bien documentada en la literatura, son escasos los reportes que describen esta entidad en pacientes con fototipos cutáneos altos.
Objetivo: presentar un caso clínico de liquen espinuloso en un paciente de piel negra.
Presentación de caso: paciente masculino de 28 años, con antecedentes de asma bronquial, que consultó por lesiones en la espalda de 2 meses de evolución. Al examen físico se observaron múltiples placas formadas por pápulas foliculares con espinas córneas centrales, ligeramente pruriginosas y de textura áspera. La biopsia cutánea mostró folículos pilosebáceos dilatados con tapones de queratina y leve infiltrado linfocitario perifolicular, hallazgos compatibles con liquen espinuloso. Se indicó tratamiento con adapaleno en gel en noches alternas y crema de urea al 10% a diario. A las 8 semanas se observó desaparición completa de las lesiones y recuperación de la textura normal de la piel.
Conclusiones: este caso confirma que las manifestaciones clínicas clásicas de liquen espinuloso se mantienen en piel negra y que el tratamiento combinado con retinoides y queratolíticos tópicos resulta efectivo. Se destaca la importancia de considerar esta dermatosis en fototipos altos, donde los reportes son escasos.
Palabras clave: Liquen Espinuloso, Queratosis Pilar, Piel Negra, Fototipo Alto, Retinoides Tópicos.
INTRODUCTION
Spiny lichen (SL) is an uncommon follicular keratotic dermatosis, considered a variant of keratosis pilaris, which occurs more frequently in children and adolescents. It is characterized by the presence of plaques formed by punctate follicular papules with central scale-like corneal spines, which give the surface a texture similar to sandpaper (1).
Its etiopathogenesis remains partially unclear; however, it has been associated with genetic predisposition and various factors suggesting a multifactorial origin. These include atopic conditions (bronchial asthma, atopic dermatitis), systemic diseases (Crohn's disease, Hodgkin's lymphoma), human immunodeficiency virus (HIV) infection, pharmacological treatments (lithium), vitamin A deficiency, as well as exposure to toxins such as thallium and arsphenamine — the latter being of merely historical interest today (2).
The typical clinical picture manifests as rounded or oval plaques of 2 to 6 cm in diameter, composed of skin-colored follicular papules with central horny projections that create a rough texture. These lesions are distributed symmetrically on the trunk, neck, shoulders, abdomen, buttocks, and extensor surfaces of the limbs, generally being asymptomatic or accompanied by mild pruritus (1-3).
Diagnosis is based on the clinical identification of characteristic plaques with follicular papules and horny spines. Dermatoscopy is a useful complementary tool, revealing multiple follicular keratotic plugs surrounded by an erythematous halo (4,5,6). Skin biopsy is conclusive, showing dilated pilosebaceous follicles with keratin plugs and a perifollicular lymphocytic infiltrate (2,3).
Regarding treatment, first-line therapy includes topical keratolytics (urea, salicylic acid, lactic acid) and topical retinoids (tretinoin, adapalene), whose mechanism of action involves the elimination of hyperkeratosis and normalization of follicular keratinization. Topical corticosteroids are reserved for cases with significant pruritus (3-5).
Although the classic presentation of SL has been widely documented (1,5), there is a notable scarcity of reports describing its semiological characteristics and therapeutic response in patients with high skin phototypes, particularly in Black-skinned individuals. This lack limits knowledge about possible clinical variations and specific therapeutic considerations in this population. Therefore, the objective of this paper is to describe a case of spiny lichen in a Black-skinned patient, highlighting its clinical particularities and the response to the established treatment.
CASE PRESENTATION
We present the case of a 28-year-old male patient, with Black skin, with a history of bronchial asthma, who attended the dermatology outpatient clinic of the General University Hospital "Calixto García". He reported the appearance of lesions on the dorsal region of approximately two months of evolution, characterized as "small bumps" that caused slight itching and a rough sensation to the touch.
Dermatological physical examination
Skin inspection revealed multiple well-defined plaques, of variable size between 3 and 6 cm, located on the dorsal region. These plaques were constituted by numerous skin-colored follicular papules, each with a protruding central horny scale in the shape of a spine, which gave the surface a rough texture similar to sandpaper (Figure 1).
Complementary studies
A 5 mm punch skin biopsy was performed, processed with hematoxylin-eosin staining. The histopathological study revealed dilated pilosebaceous follicles containing keratin plugs, accompanied by a perifollicular and superficial perivascular lymphocytic inflammatory infiltrate.
These findings, correlated with the clinical context, were compatible with the diagnosis of spiny lichen (ICD-11 code: EB90.Y Other follicular keratotic disorders). An HIV antibody detection test was requested, which was non-reactive.
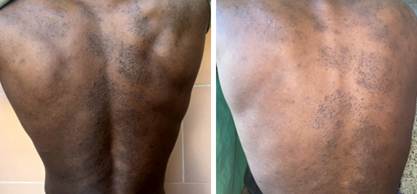
Figure 1. Multiple plaques formed by follicular papules with central horny spines, located on the back.
Treatment and evolution:
Treatment with a combined topical regimen was instituted: adapalene 0.1% gel applied on alternate nights, and 10% urea cream as a daily emollient in the mornings. At the four-week follow-up, a partial reduction of the keratotic papules and a significant decrease in skin roughness were observed. At eight weeks, complete resolution of the lesions was evidenced, with recovery of normal skin texture.
Informed consent: Written informed consent was obtained from the patient for the publication of this clinical case, guaranteeing the confidentiality of his identity by removing identifiable data.
DISCUSSION
Spiny lichen is an uncommon follicular keratotic dermatosis, considered a variant of keratosis pilaris, which predominantly affects children and young adults. Although its classic presentation is documented in the literature, there is a notable scarcity of reports describing its semiological characteristics in patients with high skin phototypes, particularly in Black-skinned individuals. The present case is relevant precisely because it documents the disease in this underrepresented population group, allowing comparisons with published series.
Clinical and epidemiological findings
Regarding the age of presentation, our 28-year-old patient falls within the described age group, although some authors, such as Venkatesh et al. (12) and Dias et al. (13), emphasize its higher frequency in childhood, while Aghighi et al. (3) report its presentation in adults. The morphology of the lesions in our patient — rounded plaques composed of follicular papules with central horny spines — fully coincides with the classic description by Antúnes-Lay et al. (8) and the cited references (1-3), confirming that the cardinal clinical picture remains regardless of skin phototype. The mild pruritus reported is consistent with that noted by Gallo et al. (1) and most authors, who describe the condition as generally asymptomatic or with minimal pruritus.
The history of bronchial asthma (atopy) in our patient is of interest, since Arora et al. (15) and the review by Aghighi (3) mention atopy as one of the associated etiological factors in this entity of unknown cause, which suggests underlying cutaneous hyperreactivity.
Diagnostic correlation
The histopathological findings observed in our case — dilated follicles with keratin plugs and a perifollicular lymphocytic infiltrate — coincide with those described by Gallo et al. (1) as conclusive criteria for diagnosis. Unlike the case reported by Aghighi et al. (3), where spiny lichen clinically simulated folliculotropic mycosis fungoides, in our patient the absence of lymphoid atypia and the favorable evolution with conventional topical treatment allowed us to firmly rule out this possibility, highlighting the importance of clinicopathological correlation.
Regarding dermatoscopy, although it was not performed in our case, Lecastre and Lopes (6) describe follicular keratotic plugs surrounded by an erythematous halo as a characteristic finding. In Black-skinned patients, where erythema may be clinically masked by skin pigmentation, this diagnostic tool takes on special relevance, constituting a limitation of our report, but also an opportunity for future research in this ethnic group.
Therapeutic approach and evolution
The treatment instituted with adapalene 0.1% and urea 10% is based on the first-line recommendations established by Gorman (4) and Sahni et al. (5), who point to topical retinoids and keratolytics as the mainstay of management. The response observed in our patient — complete resolution at eight weeks — replicates the successful results reported by Uehara et al. (10) with topical adapalene, as well as the experience of He et al. (5) with new therapeutic alternatives, although the latter used topical roflumilast with good results. Likewise, Kim et al. (14) have documented efficacy with topical tacalcitol, expanding the available therapeutic options.
Particularities in Black skin
The main contribution of our case lies in the description of spiny lichen in a Black-skinned patient, an area where Gangadhar et al. (11) and Rosamilia (7) agree on pointing out the scarcity of reports. Unlike what is observed in low phototypes, where perifollicular erythema constitutes a distinctive clinical sign (6), in our patient this finding was not evident to the naked eye, probably due to the masking conferred by skin pigmentation. However, the morphology of the papules and horny spines remained unchanged, confirming that the fundamental semiology of the disease is preserved across different phototypes.
CONCLUSIONS
Spiny lichen is a rare dermatosis that should be considered in the presence of plaques formed by follicular papules with a central spine, even in adults and in Black-skinned patients. In our case, the lesions presented the classic characteristics described in the literature, although the erythema around the follicles was less evident due to skin pigmentation. Skin biopsy confirmed the diagnosis, and treatment with adapalene and urea showed an excellent response, with complete disappearance of the lesions within 2 months. We present this case to contribute to the recognition of this disease in Black-skinned patients, a group in which there are few published reports.
BIBLIOGRAPHIC REFERENCES
1. Gallo JC, de Wet J, Visser WI, Jordaan HF, Schneider JW. Generalized lichen spinulosus and secondary follicular mucinosis. JAAD Case Rep. 2023;33:101-4. doi: 10.1016/j.jdcr.2023.01.017.
2. Gorman CR. Lichen spinulosus treatment & management [Internet]. Medscape; 2022 [cited 02/02/2026]. Available in: http://emedicine.medscape.com/article/1123533-treatment
3. Aghighi M, Pukhalskaya T, Brickley S, Smoller B. An uncommon case of lichen spinulosus in an adult patient clinically mimicking folliculotropic mycosis fungoides. Cureus. 2020;12(6):e8572. doi: 10.7759/cureus.8572.
4. Sahni VN, Dao DP, Sahni DR, Secrest AM. Lichen spinulosus: insights into treatment. Dermatol Online J. 2021;27(10). doi: 10.5070/D3271055635.
5. He R, Xu Y, Naert K, Chia JC. Successful treatment of lichen spinulosis with topical roflumilast: a case report. SAGE Open Med Case Rep. 2025;13:2050313X251400983. doi: 10.1177/2050313X251400983.
6. Lecastre A, Lopes MJ. Dermatoscopy of lichen spinulosus. An Bras Dermatol. 2012;87(6):1018-20. doi: 10.1590/S0365-05962012000600038.
7. Rosamilia L. Liquen espinuloso (queratosis espinulosa). Dermatology Advisor [Internet]. 2019 [cited 02/02/2026]. Available in: https://www.dermatologyadvisor.com/home/decision-support-in-medicine/dermatology/lichen-spinulosus-keratosis-spinulosa/
8. Antúnez-Lay A, del Barrio P, Abarzúa A. Liquen espinuloso en los codos. Piel. 2016;31(4):302-3. doi: 10.1016/j.piel.2015.09.004.
9. Ramesh H, Somashekhar S, Kanathur S. Líquenes en dermatología. Indian J Dermatol Venereol Leprol. 2023;89:908-15. doi: 10.25259/IJDVL_794_2021.
10. Uehara A, Abe M, Shimizu A, Motegi S, Amano H, Ishikawa O. Successful treatment of lichen spinulosus with topical adapalene. Eur J Dermatol. 2015;25(5):490-1. doi: 10.1684/ejd.2015.2597.
11. Gangadhar M, Adya KA, Inamadar AC. A study of clinical, dermoscopic and histopathological correlation in follicular keratotic diseases: preliminary observations in 30 cases. Indian Dermatol Online J. 2021;12(5):731-740. doi: 10.4103/idoj.IDOJ_96_21.
12. Venkatesh A, Dupuis E, Prajapati V, Rao J. Generalized lichen spinulosus in a 4-year-old boy without systemic disease. JAMA Dermatol. 2012;148(7):865-6. doi: 10.1001/archdermatol.2012.188.
13. Dias A, Santalha M, Magalhães C, Lobo AL, Pereira O. Líquen espinuloso. Acta Pediatr Port [Internet]. 2012 [cited 02/02/2026];43(5):216-7. Available in: https://ojs.pjp.spp.pt/article/download/607/2249/5957
14. Kim SH, Kang JH, Seo JK, Hwang SW, Sung HS, Lee D. Successful treatment of lichen spinulosus with topical tacalcitol cream. Pediatr Dermatol. 2010;27(5):546-7. doi: 10.1111/j.1525-1470.2010.01275.x.
15. Arora G, Khandpur S, Bansal A, Shetty B, Aggarwal S, Saha S, et al. Current understanding of frictional dermatoses: an overview. Indian J Dermatol Venereol Leprol. 2023;89:170-88. doi: 10.25259/IJDVL_519_2021.
16. Mayo Clinic. Queratosis pilaris. Rochester (MN): Mayo Foundation for Medical Education and Research [Internet]. 2024 [cited 02/02/2026]. Available in: https://www.mayoclinic.org/es/diseases-conditions/keratosis-pilaris/symptoms-causes/syc-20351149
17. Pennycook KB, McCready TA. Queratosis pilaris. En: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 [cited 02/02/2026]. Available in: https://www.ncbi.nlm.nih.gov/books/NBK546708/
AUTHORSHIP CONTRIBUTION
ARM: Conceptualization, research, data curation, methodology, visualization, drafting of the original manuscript, and revision and editing of the final manuscript.
GFG: Conceptualization, research, and supervision.
IAG: Conceptualization, research, and supervision.
APL: Conceptualization, research, and supervision.
CONFLICT OF INTEREST
The authors declare no conflict of interest.
FUNDING SOURCES
The authors received no funding for the development of this article.
USE OF ARTIFICIAL INTELLIGENCE
The authors declare that no artificial intelligence was used in the writing of this manuscript.